|
Anti-VEGF therapy with Avastin or Lucentis is considered the mainstay of treatment for myopic CNV.īevacizumab ( Avastin) is an anti-VEGF antibody that neutralises all human forms of VEGF. It is clear that ocular angiogenesis is a complex cascade that involves numerous proteins and biochemical interactions with VEGF playing a central role and its inhibition being an important therapeutic strategy. A phase II multicentre open label trial of Ranibizumab for the Treatment of Choroidal Neovascularisation Secondary to Pathological Myopia: an Individualized Regimen (REPAIR) has reported its data in 2015 and provided definitive evidence of good patient satisfaction and well-being during treatment with Ranibizumab in myopic CNV.Īnti-VEGF Therapy: The role of VEGF as a regulator of angiogenesis has been the subject of much investigation. To date one study has compared intra vitreal Avastin versus Lucentis for the treatment of myopic CNV however it found no statistical difference between both treatment arms. PDT is considered to be of limited benefit in myopic CNV. Although some improvements were shown with combination intraocular triamcinolone and PDT in patients with subfoveal myopic CNV, there were significant adverse effects associated with intra-ocular steroid (triamcinolone) use and subsequent studies have demonstrated the added effect of combination therapy to be insignificant. Photodynamic therapy (PDT) with verteporfin causes selective damage to the choriocapillaris, sparing the neurosensory retina and retinal pigment epithelium (RPE) and has been used to treat subfoveal CNV without the complications of laser photocoagulation. Myopic CNV has been treated with different approaches including laser photocoagulation, radiotherapy, submacular surgery, photodynamic therapy (PDT), ICG-mediated photothrombosis, macular translocation, combined PDT and intravitreal triamcinolone, transpupillary thermotherapy (TTT), and intravitreal injections of anti- vascular endothelial growth factor (VEGF) agents.ĭirect laser photocoagulation is of limited benefit in myopic CNV. 
Management of CNV secondary to pathological myopia The corresponding fluorescein angiograms demonstrate non specific hyperfluorescence in areas of mild atrophy of the retinal pigment epithelium and choriocapillaris (B) and intense peripapillary hyperfluoresce indicating the presence of a choroidal neovasucular membrane adjacent to extensive juxtapapillary chorioretinal atrophy (D). Thus active interventions are usually recommended for patients with myopic CNV.įigure 1 – Fundus images of 2 patients demonstrating the tessellated appearance (A), attenuated vasculature and peripapillary atrophy with associated retinal hemorrhage (C). Patients over 50 years with myopic CNV observed for a mean of 4 years had a final visual acuity (VA) of 20/200 or worse in over two thirds of cases, and a 10 year follow up observational study noted that 96% of eyes achieve a final VA of 20/200 or worse. Among myopic patients with pre-existing CNV, more than 30% will develop CNV in the fellow eye within 8 years.Īlthough natural history studies of untreated myopic CNV have presented conflicting evidence on visual prognosis, the overall trend suggests that long term visual prognosis with observation alone is poor. In its advanced stage, CNV appears as a Fuchs’ spot which is a macular scar with pigment clumping and hyperpigmentation in association with fibrosis and retinal atrophy. It is the leading aetiology of CNV among patients younger than 50 years of age. 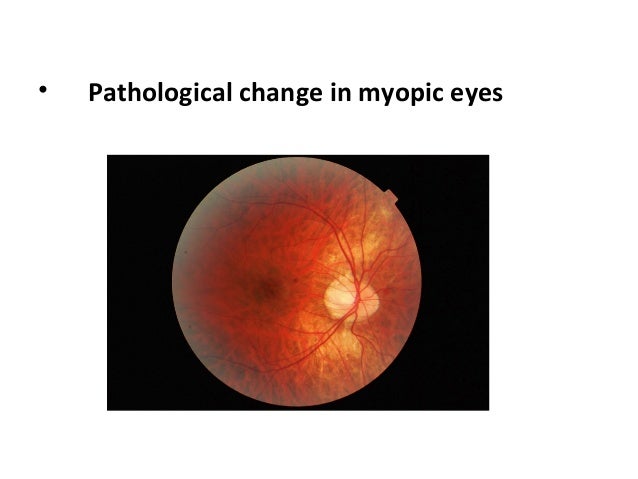
Myopic macular choroidal neovascularisation (CNV) occurs in 4% to 11% of patients with high myopia and is the most common vision threatening complication of high myopia. In addition to progressive maculopathy, macular hole, foveo-schisis and epiretinal membrane formation are much more common and often represent surgically challenging cases. Long term studies suggest that approximately 40% of highly myopic eyes develop progressive maculopathy and over ten years more than half of these individuals will lose two lines of Snellen acuity. Myopic maculopathy describes a spectrum of clinical changes that comprise the main cause of visual loss among highly myopic individuals. In the adult Asian population its prevalence is 9-21%, compared to 2.8-4.6% in the U.S and Australia and the prevalence is thought to be rising globally. The prevalence of pathological myopia (PM) is known to differ between ethnicities. 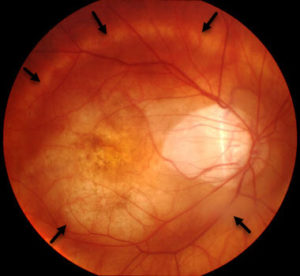
Pathological or degenerative myopia, usually defined as a spherical equivalent refractive error of ≥-6 dioptres (D) or an axial length of ≥25.5mm, is one of the leading causes of visual loss in the world. Pathological myopia – Prevalence and pathogenesis Recent trends in the management of maculopathy secondary to pathological myopia
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
